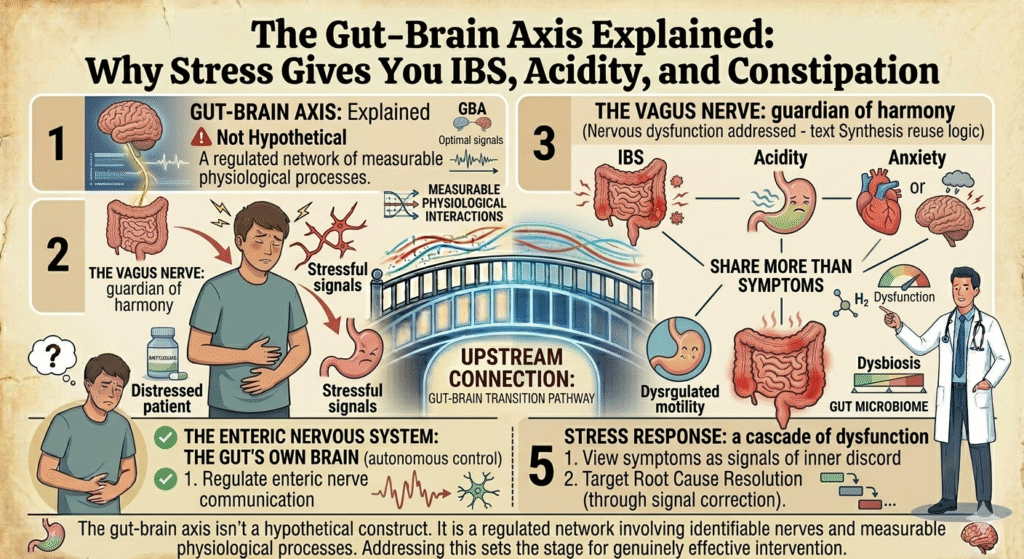
The myth of mind-body separation stubbornly persists in medical discourse, yet it is a fallacy. Stress and gut health are intertwined, rooted in the elusive yet profound gut-brain axis. Skeptics dismiss this as pseudo-medical speculation. They are wrong. The interplay between the nervous system and our digestive tract is real, observed in clinical studies and felt acutely in the symptoms of millions. Stress triggers IBS, acidity, and constipation through identifiable physiological pathways, revealing the complexity of the gut-brain connection.
Stress Alters Gut Function via the Vagus Nerve. Stress isn’t merely psychological. It manifests physically, hijacking the gut-brain axis. Central to this hijacking is the vagus nerve, the primary conduit of the parasympathetic nervous system. Chronic stress weakens vagal tone, inhibiting its regulation of digestion and peristalsis. This is not speculative. The diminished vagal activity leads to incomplete digestion and the disruption of the gut’s rhythmic contractions. The result? A surge of irritable bowel syndrome (IBS) symptoms, as well as the distressing onset of constipation a direct consequence of impaired gut motility. For those in India and beyond, understanding this crucial nerve is essential, presenting a sharp shift away from the isolated treatment of symptoms.
IBS, Anxiety, and Acidity Share More Than Symptoms. A flawed perspective reduces acidity to diet alone. Yet the nuances of anxiety, IBS, and acidity share an undercurrent a dysregulated autonomic nervous system. The hydrochloric acid production in the stomach doesn’t fluctuate by accident. It is influenced by the sympathetic nervous system’s aberrations in response to stress. Norepinephrine release increases, prompting hypersecretion of gastric acid, directly linking emotional stress to digestive chaos. The polyvagal theory further elucidates how a dominant sympathetic state inhibits the rest-digest processes. Tools for countering IBS and anxiety require explicit targeting of these neural underpinnings, challenging the oversimplified narratives that isolate gut and emotion.
The Enteric Nervous System: The Gut’s Own Brain. The enteric nervous system (ENS) operates autonomously. It comprises two sheets of neurons embedded within the gut wall, governing peristalsis and enzyme secretion. This “second brain” integrates input from the central nervous system yet functions independently, crafting a sophisticated feedback loop. Disruptions in this system, often initiated by chronic stress, alter gut motility and secretion balance, contributing to the visceral hypersensitivity seen in IBS patients. Enzymes like cholecystokinin, typically involved in fat digestion, become associated with pain perception under stress. Our understanding here reframes gut symptoms not as mere digestive issues but as expressions of complex nervous system dynamics.
The gut-brain axis isn’t a hypothetical construct. It is a regulated network involving identifiable nerves and measurable physiological processes. Stress manifests within this axis, presenting as IBS, acidity, and constipation not as psychological abstracts but as tangible clinical conditions.
Leave a Reply