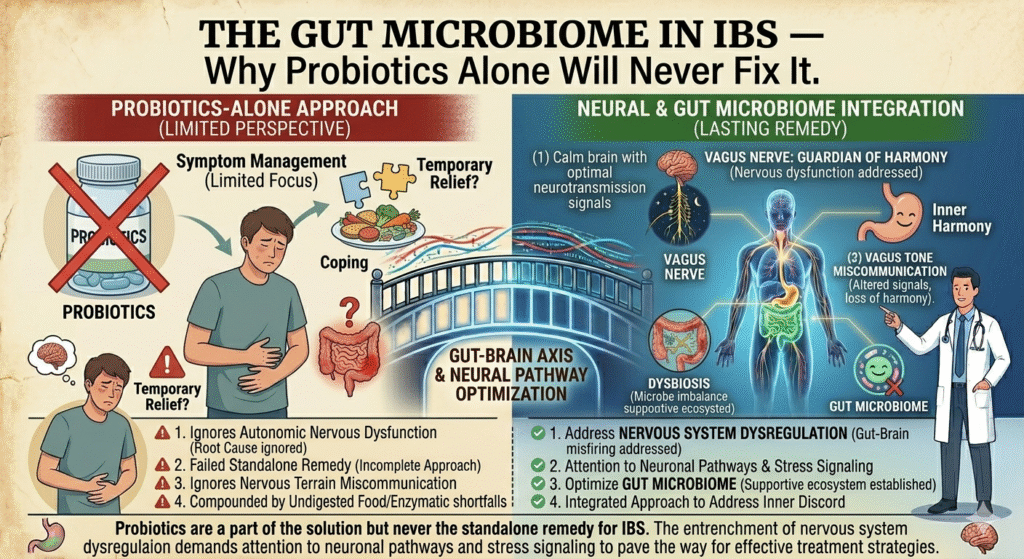
The myth is ubiquitous and misleading: Probiotics can cure IBS. This oversimplification sells products but fails to address the multifaceted nature of IBS. Probiotics alone cannot resolve unexplained gut issues. The gut microbiome is a living system influenced by the nervous system, not a one-size-fits-all supplement solution. Ignoring the interplay between gut flora and the intricate network of nerves governing our digestive processes risks leaving patients in the dark.
The Enteric Nervous System: IBS Symptomatology Beyond Bacteria
At the heart of gastrointestinal distress lies the enteric nervous system (ENS), often referred to as the ‘second brain.’ Comprising over 100 million neurons, the ENS communicates with the central nervous system via the vagus nerve. It influences digestive functions independently yet remains interconnected with our mental state. Dysfunction within this axis is at the core of irritable bowel syndrome (IBS), making it far more complex than mere gut flora imbalances. When stress triggers vagus nerve activity, it alters gut motility and secretion patterns through increased acetylcholine release. This pivotal neurotransmitter, while crucial, is often disrupted in IBS individuals. Therefore, while probiotics may modify microbial composition, they neglect the crucial ENS dysregulation.
The polyvagal theory underscores how emotional and psychological stressors can inhibit vagal tone, exacerbating gastrointestinal disturbances. Understanding IBS through this lens reveals the limitations of solely targeting bacterial colonies. Effective treatment must encompass neural regulation alongside microbial management. Patients deserve to know that IBS is not just “in their head” but directly linked to nerve signaling pathways and neurotransmitter imbalances. This complexity challenges the simplistic narrative of probiotics as a cure, demanding a more integrative approach.
Stress and the Gut-Brain Axis: A Rewiring of Misconceptions
The gut-brain axis is a bidirectional communication pathway comprising hormonal signaling, immune function, and neural circuits. Stress-based triggers via the hypothalamic-pituitary-adrenal (HPA) axis alter gut physiology when cortisol levels rise. Cortisol disrupts tight junction proteins like zonulin, increasing intestinal permeability. Such changes precede microbiome imbalance. Thus, the psychosomatic influence cannot be understated. Reducing the microbiome relationship to probiotics disregards the stress-induced shifts in gut function that precede microbial dysbiosis.
This cascade effect highlights the limitations of addressing IBS without considering the gut-brain interplay. While a healthy microbiome can mitigate stress response, it does not tackle the root stressors affecting neurotransmitter and hormone regulation that aggravate IBS symptoms. To resolve unexplained gut issues, clinicians must identify the neural mechanisms amplifying stress responses, not just adjust bacterial counts. The fixation on probiotics falls short of modifying the stress-sensitive gut environment supervised by the CNS.
Nervous System Dysregulation: Beyond Bacterial Realms
Gastrointestinal functionality and the nervous system coexist in a state of delicate balance. The neurotransmitters serotonin and norepinephrine, predominantly produced in the gut, illustrate the profound impact of the nervous system on digestion. These biochemical messengers modulate gut motility and visceral sensitivity, both compromised in IBS. Disturbances in neural communication pathways lead to hypersensitive pain responses and erratic peristalsis. Attempting to remedy this with probiotics alone is clinically insufficient.
Given the intertwined nature of neurotransmitter production and gut microbiome integrity, addressing IBS necessitates an understanding of the neurotransmitter biosynthesis pathway within the gut-brain axis. The body’s inability to normalize neurotransmitter levels in the presence of psychosocial stressors reveals the neural disruption underpinning IBS. It is not a simple matter of repopulating symbiotic bacteria but involves recalibrating the entire neuro-digestive network to normalize digestive processes.
Probiotics are a part of the solution but never the standalone remedy for IBS. The entrenchment of nervous system dysregulation demands attention to neuronal pathways and stress signaling to pave the way for effective treatment strategies. This multifactorial perspective offers the clinical precision necessary for navigating the complexities of IBS beyond simplistic remedy myths.
Leave a Reply