You’ve been told that chronic constipation is simply about dietary fiber and water intake. A persistent myth perpetuated by an outdated medical narrative. Chronic constipation is not just about what you eat. It’s a complex issue deeply tied to the intrinsic mechanisms of your gut, including the migrating motor complex (MMC), a remarkable internal cleaning system, often overlooked. This process is not fuelled by nutrients but by a sophisticated, wave-like motion that sweeps through your intestines. It acts almost like a nighttime janitor for your digestive tract, ensuring waste and bacteria are kept in check. Many healthcare providers neglect this crucial aspect of gut health, a significant oversight for those struggling with incomplete evacuation.
Unveiling the Migrating Motor Complex: Your Gut’s Immune System
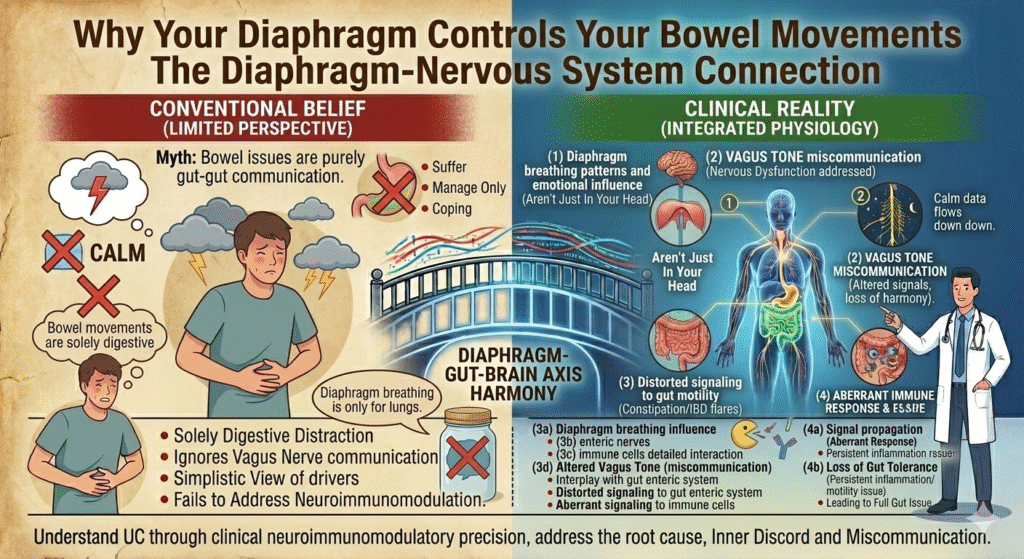
The migrating motor complex is an electrochemical signal, initiated by the enteric nervous system, that orchestrates your gut’s intrinsic housekeeping. This system operates independently from conscious thought, regulated by motilin, a hormone secreted by the enterochromaffin cells in the small intestine. During fasting, the MMC is triggered every 90 to 120 minutes, propelling indigestible substances and bacterial overgrowth toward the colon, embracing the concept of ‘cleansing cycles.’ A disruption here often correlates with chronic constipation. Remember, the brain’s blueprint of health does not always align with reality. When the MMC falters, the nervous system becomes compromised. Control is asserted by the vagus nerve, the bridge between your brain and gut. This nerve’s functionality, or dysfunction, is critical in understanding ongoing digestive issues. If the vagus nerve is dysregulated, so too is the migrating motor complex. Once this connection is established, a comprehensive understanding of chronic constipation emerges, deviating from simplistic advice about fiber and fluid intake.
The Gut-Brain Axis: Chronic Constipation’s Neural Backdrop
The vagus nerve plays a leading role within the gut-brain axis, a communication superhighway between your central nervous system and enteric nervous system. Polyvagal theory elucidates this process further, highlighting the interaction between emotional states and physiological responses. Stress, anxiety, and other emotional patterns can impair vagal function, leading to internal chaos. Here lies a fundamental truth: digestion is as much a neurological process as it is biological. The gut’s neurons, sometimes called the ‘second brain,’ are not a static bystander. They actively modulate the MMC. Impaired vagal tone directly affects gut motility, resulting in the encumbrances of chronic constipation and incomplete evacuation. No doctor asks about your parasympathetic state during a ten-minute consult, yet it dictates everything from your heartbeat to bowel movements. Once you grasp this, the resolution of chronic constipation through neural pathways, rather than dietary adjustments, becomes evident.
Pathophysiological Insights: The Junction of Dysfunction
Exploring the cellular architecture of the gut reveals complex enzymatic pathways at play. Consider the role of cholecystokinin (CCK) and serotonin in conjunction with the MMC. These neurotransmitters and hormones fine-tune digestive motility and appetite regulation. Serotonin, although primarily associated with the brain, exists predominantly in the gut, precisely fine-tuning peristalsis and MMC functioning. A disruption here, whether due to receptor sensitivity or secretion levels, impedes the MMC’s operation, leading directly to chronic constipation. This is not a dietary fiber issue; this is a neurotransmitter imbalance. For those branded with ‘irritable bowel syndrome,’ knowledge of these neural pathways is poorly disseminated. Understanding that the intrinsic regulation of bowel movements is neurogastroenterological not dietary in origin is a revelation that redefines earlier misconceptions.
Understanding chronic constipation demands a shift in perspective, acknowledging the gut’s neurophysiological underpinnings rather than adhering to outdated nutritional advice. It’s the migrating motor complex, this unsung hero of gut health that maintains internal harmony. A failure here, correlated with vagal nerve dysfunction and neurotransmitter imbalances, redefines what you thought you knew about digestion. A sound clinical foundation reorients diagnosis and treatment strategies, illuminating pathways far more intrinsic than superficial dietary changes. Chronic constipation is not solved in the kitchen it’s resolved in the neurology of your gut.
Meta Description: Chronic constipation isn’t about fiber; it’s the migrating motor complex, a neglected gut nerve network set by neurogastroenterological dynamics.