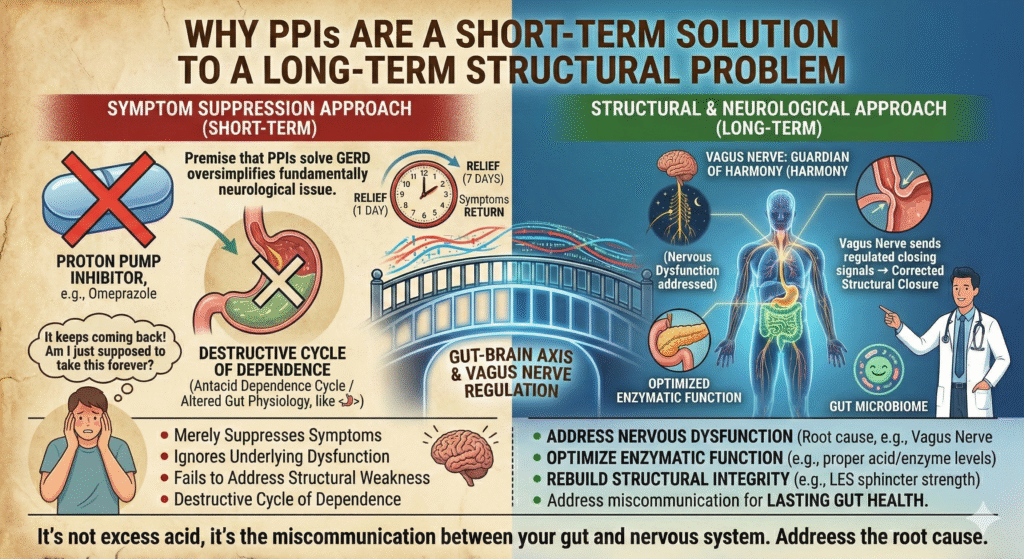
Myth: Acid reflux is merely an issue of excess stomach acid easily managed with medication. False. This simplistic view ignores the underlying complexities. Stomach acid isn’t the enemy; it’s often a scapegoat. Proton pump inhibitors (PPIs) offer temporary relief but fail to address root structural imbalances. Acid reflux is more than just acidity it’s a symptom of a misaligned internal network involving your nervous system, notably the vagus nerve.
The Nervous System’s Impact on Gut Health: A Clinical Analysis
Acid reflux, bloating, and related symptoms extend beyond gastric mechanics. The vagus nerve a cornerstone of the nervous system plays a significant role in modulating gastrointestinal function. When you swallow, the vagus nerve stimulates gastric acid production. An out-of-sorts nervous system can malfunction here, amplifying or muting this signal, culminating in gastrointestinal issues. Excessive use of PPIs disrupts this neural pathway further, impairing your enteric nervous system’s innate regulation. Moreover, nervous system dysregulation can trigger acidic imbalance, bloating, and inflammation. The problem isn’t your body producing too much acid; it’s that neural networks governing acid balance are misaligned. Recognizing this shifts the focus from chemistry to neurophysiology, reframing your understanding of downstream symptoms.
PPIs: A Temporary Fix with Long-Term Costs
Proton pump inhibitors do more harm than good over time. Initially, they provide a false sense of security by reducing stomach acid, seemingly resolving acidity and bloating. Unfortunately, continued PPI usage alters vital enzymatic processes like pepsinogen conversion. This can compromise nutrient absorption and disrupt microbiome balance. Diminished stomach acidity due to excessive antacid use fosters bacterial overgrowth, setting the stage for further complications. Ironically, the reflux persists or worsens over prolonged usage as the stomach becomes dependent on the medication rather than restoring its natural regulatory function. Relegating acid reflux management to PPIs keeps the root neural imbalance intact. True resolution lies in correcting the nerve pathways and enzymatic cascades that regulate your gut.
The Gut-Brain Axis: Where Emotions and Acid Reflux Intersect
The relationship between the gut and brain is bidirectional. Emotional patterns can trigger reflux by influencing the gut-brain axis. Polyvagal theory provides insight into this interaction. High levels of stress or trauma can lock the vagus nerve in a sympathetic dominant state, disturbing gastrointestinal motility and acid regulation. This triggers or exacerbates reflux symptoms. Medications like PPIs don’t address this neurobiological interplay. A clinical understanding recognizes these symptoms as the body’s response to neural and emotional data, not merely excess acidity. Reframing this interaction reveals the real culprit: nervous system dysregulation confounding normal digestive processes.
The premise that PPIs solve acid reflux oversimplifies a fundamentally neurological issue. The clinical path acknowledges that lasting gut health requires addressing nervous and enzymatic dysfunction rather than merely suppressing symptoms. It’s not excess acid it’s the miscommunication between your gut and nervous system.