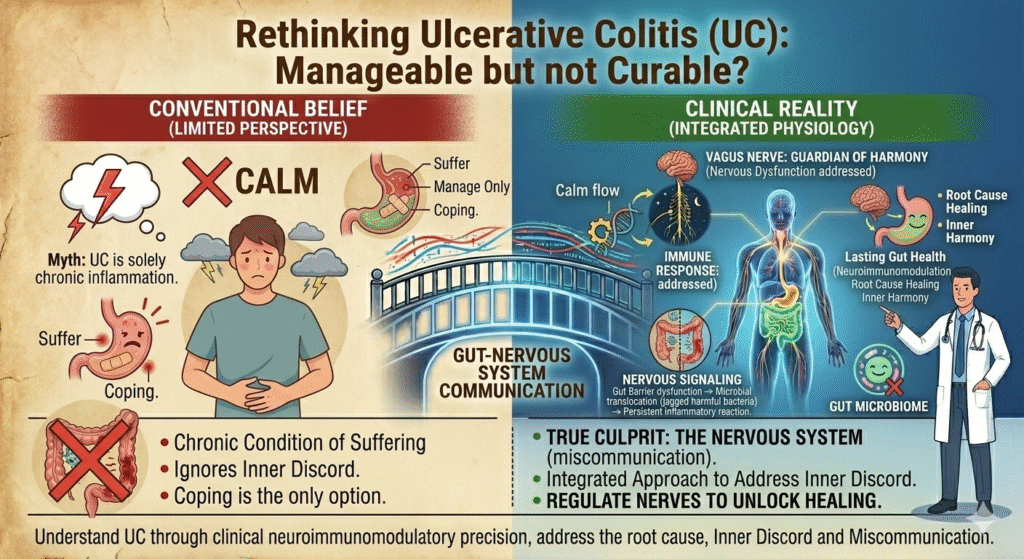
Modern medicine sells you a lie – ulcerative colitis is manageable but not curable. A chronic condition you must suffer and cope with indefinitely. This belief fails to mention the true culprit: the nervous system, intricately involved in Inflammatory Bowel Disease (IBD). While standard care focuses on symptom suppression, it overlooks critical pathways like the vagus nerve and their role in symptom perpetuation. IBD is more than an unmanaged immune response in the colon; it’s a miscommunication within your entire autonomic landscape.
Failure of Predictive Medicine
The current model of ulcerative colitis management is a reactive approach, primarily focused on symptomatic medication to tame inflammation. Mesalamine might soothe, and corticosteroids might quell a flare, but what about the cellular mechanisms? The standard practice ignores the enteric nervous system a vast network containing neurotransmitters like serotonin that rival the brain’s complexity. The gut’s serotonin is not mere decoration; it governs intestinal motility, sends feedback to the central nervous system, and modulates inflammatory pathways. The failure to correct serotonin imbalance perpetuates the cycle of intestinal dysfunction.
Completed evacuation is a fundamental measure, yet “incomplete evacuation” plagues those with ulcerative colitis, a result of misfiring neuromuscular and neuroimmune signals. The gut-brain axis, more than just a trendy term, describes a highway of neural conversation where misregulated signals can amplify IBD symptoms. Medications wear a Band-Aid over a nerve that screams for tuning. Understanding this conversation re-defines how ulcerative colitis is managed beyond symptomatic relief to neuromodulation.
Immune Dysregulation Beyond the Gut
It isn’t just the gut that’s on fire in ulcerative colitis. The enteric nervous system modulates immune cells like T-regulatory and Th17 cells, which wield influence over inflammatory stimuli. When the polyvagal theory comes into play, we’re talking about the dual functionality of your vagus nerve both calming inflammation and influencing heart rate variability that contributes to emotional regulation. In states of dysregulation, systemic inflammation isn’t confined to the gut. Patients often report anxiety, a hyperawareness brought on by a nervous system constantly on alert.
The standard model does not address lymphoid aggregates or Peyer’s patches, pivotal in the interplay between the digestive and immune systems. The unchecked dominance of pro-inflammatory cytokines only fuels an immune aggressor that has lost its way. The oversight of immunological dialogue leaves patients suspended in a pseudo-state of health where the inflammatory storm is diminished, not dispersed. The immune response is not merely a cascade but a complex, multi-channel conversation that requires tuning into neural feedback.
Nervous System Hypersensitivity and Emotional Patterns
Split-second decisions by your autonomic nervous system determine whether you digest, sleep, or defend. In individuals with ulcerative colitis, these decisions are skewed, often favoring defense. Cue the minor stressors that mount, triggering cortisol spikes more befitting a battlefield than daily life. The dysfunction isn’t psychological; it’s neurological, involving pathways like the hypothalamic-pituitary-adrenal (HPA) axis caught in a feedback of over-response.
The emotional landscape is marinated in biochemical reality. Gut-biased production of neurotransmitters such as GABA and dopamine directly affects mood and intestinal motility. The standard model often misclassifies anxiety or depression as secondary, yet for ulcerative colitis, these emotional patterns are a byproduct of a hyped nervous system. Without understanding how autonomic neuropathways contribute to these perceptions, treatment remains myopic at best.
Embracing neural mechanisms is not just about gut health; it’s redefining how conditions like ulcerative colitis are witnessed and addressed. An imbalanced nervous system dictates an imbalanced gut. The standard medical paradigm must contend with this reality or concede the illusion of true resolution. A neurological understanding turns the page, allowing clearer insights and expanded pathways for intervention beyond mere management.
**Meta Description:**
Managed, not resolved ulcerative colitis remains an IBD mystery within the standard model. The truth resides in the unexplored neural conversations.