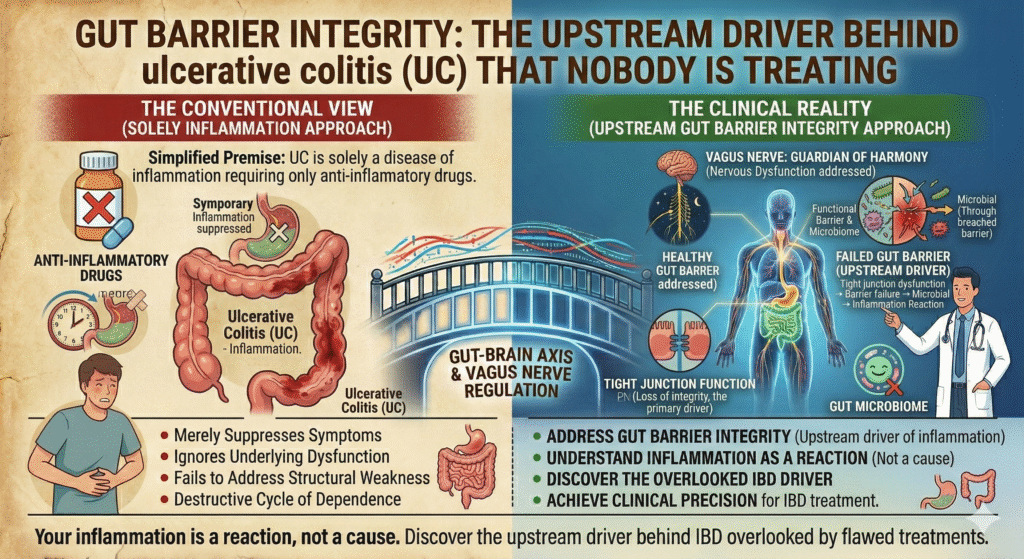
Let’s dispel a persistent myth: ulcerative colitis (UC) is solely a disease of inflammation requiring only anti-inflammatory drugs. The truth? Ineffective focus. Inflammatory Bowel Disease, or IBD, needs upstream intervention where the gut barrier integrity is the unsuspecting culprit. This elemental dysfunction perpetuates the cycle of inflammation your standard treatment fails to address. Your immune system isn’t misbehaving; it’s reacting predictably to a compromised barrier.
**The Pathophysiology of Gut Barrier Dysfunction**
The gut barrier is a sophisticated and critical defense line, not a passive boundary. Held together by proteins like occludin and claudins, the tight junctions seal the intestinal lining, preventing unwanted intruders. Failure of this barrier leads directly to an orchestrated chaos known as increased intestinal permeability, often termed ‘leaky gut.’ Here lies the upstream problem in UC, not the downstream symptoms of its consequences. The translocation of luminal antigens, bacteria, and toxins ignites a chronic inflammatory response. This breach is not merely a breach; it is the ignition of a pathological feedback loop.
If the tight junction barrier falters, the immune system perceives relentless provocation. Regulatory T cells are overwhelmed, unable to deactivate the constant alerts sounded by dendritic cells encountering misplaced antigens. Resultant pro-inflammatory cytokines like TNF-alpha and IL-6 perpetuate a damaging cycle. Disrupted immune tolerance becomes the norm. Your intestines aren’t just inflamed; they’re under siege. It’s this breach that’s ignored in conventional treatments focused myopically on symptom suppression.
Your understanding pivots here: gut barrier failure drives UC, not inflammation itself. Conventional medicine treats the symptom, not its upstream origin.
**Enteric Nervous System: The Unsung Conductor**
Neglect of the enteric nervous system (ENS) is as egregious as it is common. This ‘second brain,’ formidably autonomous, coordinates digestion, modulates local immune responses, and maintains mucosal integrity. The neglected factor in UC is the dysfunctional ENS, inducing changes that confuse its direct communication line with the central nervous system via the vagus nerve. Polyvagal theory explains further; the vagus nerve especially its dorsal pathway mediates anti-inflammatory reflexes that are hacked in UC patients.
ENS compromise starts to modify gut motility, evident in the distressing symptom of incomplete evacuation many UC patients endure. Aberrant signaling via the vagus nerve leads to sympathetic dominance, exacerbating gut permeability and muscular miscoordination. This is not psychosomatic; this is cellular communication run amok. ENS dysfunction, peripheral to gut barrier integrity, exacerbates the disease state.
Discover a pivotal truth: the gut-brain axis functions as a bidirectional highway dictating your gut’s fate, where neural dysfunction multiplies IBD complexity.
**Destructive Inflammation: A Misunderstood Reaction**
Now, let’s strip away the prevailing misconception: inflammation in UC is exclusively due to autoimmunity gone rogue. An inaccurate oversimplification. The chronicity of UC-related inflammation finds its roots in microbial dysbiosis, enhanced epithelial permeability, and failing mucosal repair areas virtually unexamined by current treatments. The enemy is not natural immune aggression; it’s the inappropriate focus on symptoms rather than pathways of initiation. Your immune system’s ‘mainstream villainy’ is, in reality, your body’s war against an unseen bacterial translocation stemming from gut barrier failure.
Understanding the mechanism unfurls another layer; MAPK and NF-kB pathways are activated by this microbial intrusion. These signaling cascades drive cytokine storms that are amplified by dysregulated paneth cells unable to adequately mount mucosal defenses. You lament inflammation, yet it is the body’s desperate cue for restoration ignored by treatments stuck on downstream suppression through biologics and steroids.
Redirect your lens: the inflammatory cascades in UC are self-compounded responses to systemic neglect of a porous gut barrier. Your disease is not an inflammatory anomaly; it is an escalated consequence.
Key insight ignored by typical therapeutic regimens is this: the integrity of the gut barrier determines the course and severity of UC. Standard treatments overlook this upstream factor, fixating instead on downstream inflammations. Elevate your understanding. Demand upstream treatment of your UC for tangible remission.
**Meta Description:**
Gut barrier integrity fails in UC. Your inflammation is a reaction, not a cause. Discover the upstream driver behind IBD overlooked by flawed treatments.