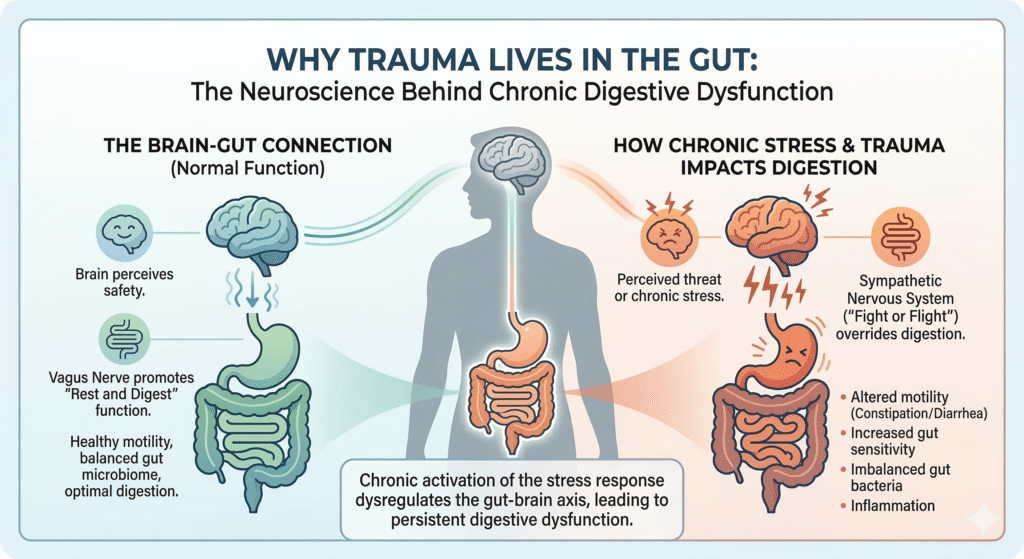
The myth that your gut issues are all about diet needs annihilation. Yes, what you eat matters, but the mere focus on diet overshadows the invisible forces within your nervous system. Trauma often lodges itself in the gut due to the intricate interplay between emotional stressors and physiological responses modulated by the gut & nervous system. The gut-brain axis is not a buzzword; it’s a scientifically grounded concept crucial to understanding chronic digestive dysfunction.
**Vagus Nerve: The Gateway of Gut and Nervous System Interaction**
The vagus nerve: a crucial player. It’s responsible for the bi-directional communication between the brain and gut. When trauma occurs, this communication can become dysregulated. The vagus nerve, as a major component of the parasympathetic nervous system, modulates stress responses. Emotional trauma desynchronizes vagal tones, causing gastrointestinal distress. Physiology adds gravity: low vagal tone results in diminished acetylcholine release, impairing gut motility and secretion of digestive enzymes. Polyvagal theory expands on this. It asserts that our autonomic nervous system, pivoted by the vagus nerve, adapts to perceived threats real or imagined. Chronic overactivation prepares the gut to fail. Trauma occasionally hijacks this adaptive mechanism, embedding dysfunctional patterns in the digestive tract.
Herein lies the truth: Trauma’s legacy lives in vagal pathways and not merely the physical scars.
**Enteric Nervous System: Your Second Brain Holding Trauma Hostage**
The enteric nervous system (ENS) is compelling evidence for why trauma sticks in the gut. Sometimes called the “second brain,” the ENS contains over 100 million neurons in the gastrointestinal tract. Its autonomous nature illustrates how gut disorders can persist independently of conscious thought. Stress-traumatically induced neuroplasticity reshapes neural circuits in the enteric system, tearing apart normal digestive function. Traumatic experiences often result in altered serotonin signaling within the ENS, as serotonin is implicated in motility and secretion. Disrupted serotonin pathways lead to symptoms classic to irritable bowel syndrome, a condition often correlating with trauma history. Furthermore, heightened cortisol levels from prolonged trauma exposure amplify inflammatory cytokines in the gut scrambling normal gut-brain axis signals.
Understand this reality: Your gut is a neural vantage point for trauma, as real as any cognitive dysfunction.
**Gut-Brain Axis: The Direct Conduit of Trauma-Driven Dysregulation**
The gut-brain axis is not just an anatomical corridor. It’s the crucial dialogue your trauma exploits. Consider microbiota dynamic ecosystems producing metabolites influencing both gut biomechanics and neurobehavioral outcomes. Traumatic stress reconfigures this microbial landscape, fostering environments for harmful bacteria. This microbial imbalance triggers immune responses, releasing substances like lipopolysaccharides that alter brain function. Traumatic memory and gut dysbiosis are interwoven through altered hypothalamic-pituitary-adrenal (HPA) axis activity. The result? Persistent miscommunication through the vagus nerve culminates in digestive symptoms. Dysregulation of the HPA axis post-trauma becomes a tangible disruptor of digestive equilibrium, confirming that trauma reroutes biological mechanisms you cannot consciously control.
The takeaway: Trauma places roadblocks in the regulatory highways of your gut-brain axis it’s not “just stress.”
Your gut, invaded by trauma, is an authoritative narrative. This isn’t conjecture based on emotional wellness; it’s the orchestration of neural pathways, neurotransmitters, and physiological response relentlessly scientific. The gut & nervous system is a battleground where trauma manifests, breeds, and perpetuates chronic dysfunction in stark defiance of superficial solutions. Your symptoms are the soundless echoes of trauma’s persistence.