Let’s dismantle a myth. Chronic stress isn’t just a mental affliction. The cliché that stress is purely psychological and only heightens anxiety misleads and misinforms. Chronic stress unleashes a cascade of physiological disruptions, with the gut bearing the brunt. Chronic stress affects the gut and nervous system, essentially obstructing digestion.
Chronic Stress Paralyzes Your Vagus Nerve
The medical community often overlooks the vital role of the vagus nerve in the gut-brain axis. This nerve connects the brain stem to the gut, operating as the body’s telecommunication line. When stress intensifies, the body’s stress response suppresses the vagus nerve’s ability to function. This process, known as impaired vagal tone, dictates how well your gut manages to process food. It’s not your mind playing tricks; it’s a tangible failure of your body’s neural wiring.
There’s no shortage of evidence linking chronic stress to impaired digestion through the vagus nerve. High cortisol levels, born from relentless stress, deplete acetylcholine the neurotransmitter facilitating vagal communication. A disruption in this pathway leads to decreased gastrointestinal motility. Enteric nervous system dysfunction sets in, breeding conditions like irritable bowel syndrome. You never heard it from your doctor, but when your stomach’s churning, cortisol and a stifled vagus nerve are largely responsible.
Neuroscience Redefines Emotional Stress Through Digestive Impact
We venture beyond psychology when examining stress impacts. Neuroscience elucidates on the interplay between stress, the nervous system, and digestion. The gut-brain axis becomes a battlefield under stress. Here, the enteric nervous system, constituting a ‘second brain,’ wields control over gut function. Yet, under stress’s tyranny, this sophisticated network falters.
Stress infiltrates this axis, triggering neuroinflammatory responses and altering gut microbiota. Glutamate receptors flood the system due to stress, agitating enteric neurons, and further compromising motility and digestion. Past your physician’s myopic view, enter a scenario where emotional imbalances birth gut imbalances through raw, biochemical interference. The gut-brain axis is not a mere abstract; it is the very neurological lifeline under siege.
Polyvagal Theory Lays Bare the Digestive Toll of Stress
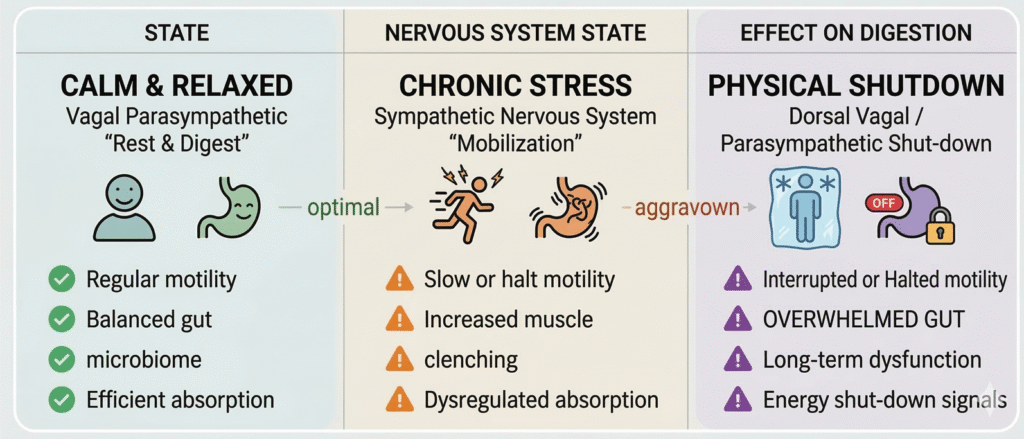
Polyvagal theory, introduced by Dr. Stephen Porges, offers a revolutionary lens through which we understand stress’s impact on digestion. This theory unveils the dual role of the vagus nerve, also considering the physiological state of safety and social engagement the optimal state for digestion. Under chronic stress, the system is hijacked, stranding the body in constant fight or flight. Digestive processes? Completely sidelined.
In this state, vagal braking of the heart reduces, diverting blood from digestive organs. A shift occurs towards a sympathetic dominance, halting secretion of crucial digestive enzymes like pepsin and the reduction of gastric acid production. These biochemical shifts are not just collateral stress damage; they are indicators of a systemic collapse rooted in neurophysiological principles. Going forward, understanding these principles redefines your view of chronic stress not as an abstract anxiety but as a direct debilitator of gut function.
Stress doesn’t just twist your thoughts; it twists your gut into knots. The enteric nervous system, gut-brain axis, and polyvagal theory expose chronic stress’s true nature. Misunderstood and mishandled by many, this knowledge is pivotal. Clinical truth: your gut doesn’t just feel stress, it breaks under its pressure.