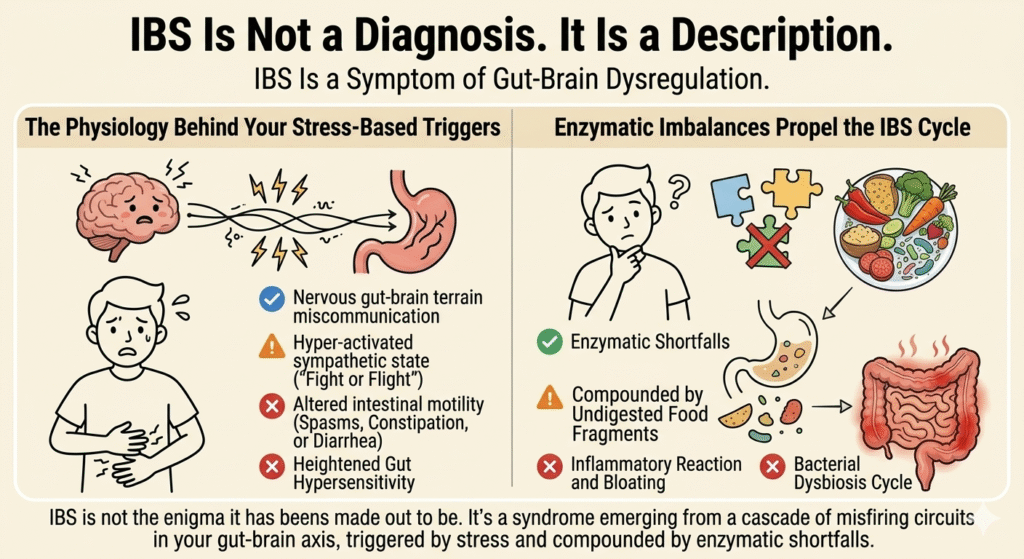
Let’s destroy a common misconception: Irritable Bowel Syndrome (IBS) is not a diagnosis; it is merely a description of symptoms. When you are told you have IBS, it’s simply a label attached to your unexplained gut issues. It does not reveal what’s truly malfunctioning within the labyrinth of your gut-brain axis. Calling IBS a diagnosis absolves the medical model from digging deeper into the physiological disruptions taking place. This is why patients continue to suffer without real answers.
IBS Is a Symptom of Gut-Brain Dysregulation
The phrase “unexplained gut issues” is misleading. The real culprits lie in the miscommunication between the gut and brain, specifically through the vagus nerve. The vagus nerve serves as a key mediator in the gut-brain axis, a complex circuitry involving the enteric nervous system and central nervous system. Vagus nerve dysfunction can lead to dysbiosis a microbial imbalance that triggers many IBS symptoms. Understanding the impact of vagal tone, or the level of activity within the vagus nerve, is crucial. A lower vagal tone is associated with a higher likelihood of IBS symptoms due to impaired gut motility and secretion.
Gut-brain communication is not speculative; it is biological fact. Dysfunction along this axis can provoke intestinal permeability and an overactive immune response. When the vagus nerve fails to regulate, the enteric nervous system falls into a state of chaos, manifesting as IBS. This dysfunction is exacerbated by stress-based triggers, including cortisol spikes and autonomic nervous system imbalances. The reality: IBS is a symptom of a malfunctioning gut-brain dialogue, not a standalone disease.
The Physiology Behind Your Stress-Based Triggers
Stress is often brushed aside as a vague contributor to IBS. But stress initiates specific biochemical pathways that escalate the issue. The corticotropin-releasing factor (CRF) plays a pivotal role here, exacerbating gut motility and secretion through neural pathways. When stress activates CRF, it prompts a cascade of reactions leading to visceral hypersensitivity. You don’t just “feel stressed,” your gut transmits that stress as concrete symptoms. The HPA (hypothalamic-pituitary-adrenal) axis further disrupts gastrointestinal processes by chronic release of cortisol, leading to altered gut permeability.
Polyvagal theory offers insights into this puzzle, highlighting how autonomic nervous system responses to perceived stress contribute to gut inflammation and dysbiosis. The sympathetic nervous system’s overactivation can perpetuate a feedback loop of stress and physical symptoms, forcing you further into the grip of IBS episodes. Each stress cue isn’t just emotional; it’s biochemical, influencing serotonin and other neurotransmitters in the gut. This elucidates why pharmaceutical interventions aimed at symptomatic relief fail to address the physiological malfunction. Here’s the truth: Your “stress” isn’t just in your head; it’s embedded in your gut.
Enzymatic Imbalances Propel the IBS Cycle
IBS isn’t just a nervous system malfunction; it’s also driven by enzymatic imbalances. Lactase deficiency, for instance, isn’t merely a dietary inconvenience but a trigger for fermentation and gas production, heightening IBS symptoms. Sucrase-isomaltase deficiencies can similarly wreak havoc, disrupting the digestion of carbohydrates and promoting gut inflammation. When enzymes that should break down specific foods are absent or dysfunctional, it results in a mechanical failure of the digestive process. This doesn’t go unnoticed; it adds fuel to the already burning fire of inflammation and immune response in the gut.
Maldigestion doesn’t only affect nutrient absorption; it directly impacts the mucosal immune system, provoking an inflammatory response. Enterocytes, the intestinal lining cells, react to these enzymatic disruptions by altering tight junctions, further compromising gut integrity. The truth is, IBS patients aren’t just dealing with errant nerves; they face systemic digestive failure underpinned by biochemical insufficiencies.
IBS is not the enigma it has been made out to be. It’s a syndrome emerging from a cascade of misfiring circuits in your gut-brain axis, triggered by stress and compounded by enzymatic shortfalls. Dispelling the IBS myth reveals a complex interplay of neural, hormonal, and enzymatic disruptions. Your symptoms are not inexplicable; they are a clarion call to investigate deeper biological truths. Understanding IBS requires abandoning misconceptions and acknowledging the precise, albeit underdiagnosed, physiological processes at play.