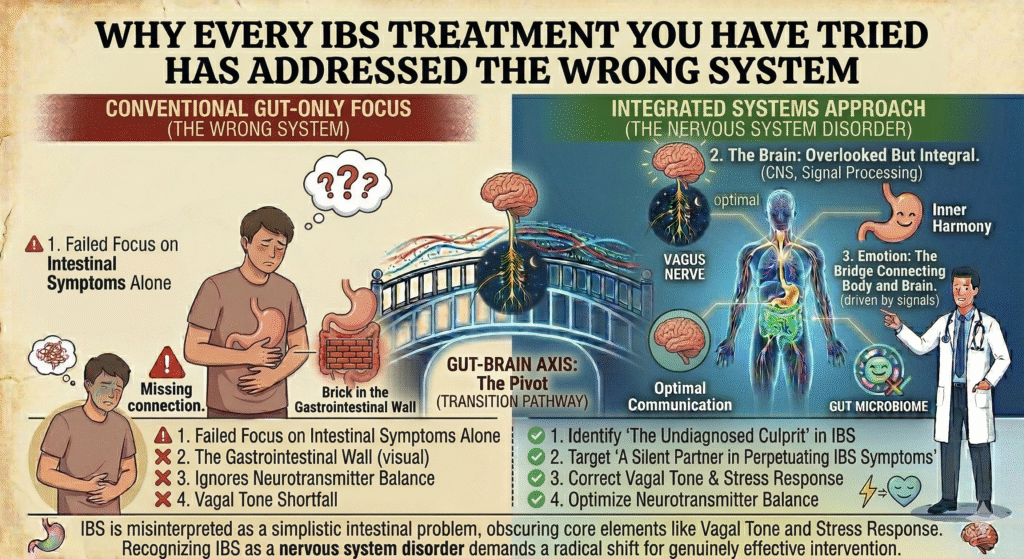
The myth of isolated gut treatment for IBS is pervasive. Dietary changes and medications often chase symptoms, leaving the real causative systems untouched. Treatments focused exclusively on the gastrointestinal tract fail because they ignore the intricate dance between the gut and the nervous system. IBS is a disorder rooted not just in digestive dysfunction, but also in the central regulation mediated by your nervous system’s master conductor the vagus nerve.
The Enteric Nervous System: More Than Just a Brick in the Gastrointestinal Wall
The enteric nervous system is not merely a subordinate to the brain; it is a self-regulated entity often termed the “second brain.” It operates on the axis of your entire digestive tract. The crux of misunderstanding lies in a narrow perspective that pigeonholes IBS as merely gut-centric. The intricate network of neurons lining your intestines constantly communicates with your central nervous system through the gut-brain axis. This is not a simple call-and-response system but a bidirectional network where signals are transmitted via the vagus nerve. Over 90% of its fibers are afferent, meaning they send information from your gut to your brain. Serotonin, predominantly found in the gut, modulates not just mood, but also gastrointestinal motility. Your gut issues might very well be a misfire in neurotransmitter signaling rather than just a digestive malfunction.
Stress-based triggers further exacerbate this dysfunction. Corticotropin-releasing hormone (CRH) secreted during stress episodes impacts gut permeability and motility, perpetuating IBS symptoms. Conventional treatments fail to address these neuroendocrine disruptions, thus bypassing a foundational element of your condition. Reframe IBS as not just a gut ailment but a disorder of neural signaling and stress response.
Nervous System Dysregulation: The Undiagnosed Culprit in IBS
IBS treatment often focuses myopically on dietary or pharmaceutical interventions. This overlooks the fundamental issue: a dysregulated autonomic nervous system. The polyvagal theory, introduced by Stephen Porges, elucidates how the vagus nerve mediates stress responses. This includes shifting between the parasympathetic and sympathetic states. In individuals with IBS, there’s often a skew towards sympathetic dominance, also known as the fight-or-flight response. This imbalance can perpetuate severe discomfort, pain, and bowel irregularities.
Key physiological processes, such as reduced vagal tone, demonstrate the impact of nervous system dysregulation. A lowered vagal tone has been correlated with diminished communication between the gut and the brain, affecting both immune function and gut barriers. Addressing IBS without considering these elements ensures the continuation of unexplained gut issues. The misalignment is not simply digestive it is a systemic failure of neural integration.
Neurotransmitter Imbalance: A Silent Partner in Perpetuating IBS Symptoms
Neurotransmitter imbalances are notorious but overlooked contributors to the persistence of IBS. Not just serotonin, but dopamine and acetylcholine play roles in gut functionality. Dopamine’s influence on motivation extends to promoting motility, while acetylcholine’s role, mediated by the vagus nerve, impacts gastrointestinal secretion and muscle contraction. The enzyme monoamine oxidase’s activity is critical here; altered levels can disrupt the balance, leading to uncoordinated muscle contractions or ‘spasms’ typical of IBS.
Furthermore, immune responses in the gut, heavily modulated by neurotransmitters, can propagate inflammatory pathways. This adds another dimension of complexity to gut symptoms. Without rectifying these neurochemical imbalances, treatments inadvertently miss the target. Recognize IBS as an interaction of neurotransmitter dysregulation and nervous system imbalance, not just an isolated gut issue.
IBS is often misrepresented as a simplistic intestinal problem. This erroneous focus has obscured the core elements that perpetuate symptoms, such as vagal tone, neurotransmitter balance, and stress responses. The gut-brain axis is a pivotal neural pathway that transcends traditional digestive treatment, demanding a radical shift in understanding. Recognizing IBS as a nervous system disorder sets the stage for genuinely effective intervention.