There is a pervasive myth in modern medicine that chronic digestive conditions stem solely from gut-related issues. This myth is perpetuated by a healthcare system focused more on symptomatic relief than on finding the root cause. The truth is more complex. Gut symptoms often have their origins not in the gut itself, but in the interconnected networks of the gut, the nervous system, and emotional patterns. Recognizing this, the gut & nervous system’s interdependence becomes the key to understanding and effectively treating chronic digestive conditions that remain unmanaged by conventional medical approaches.
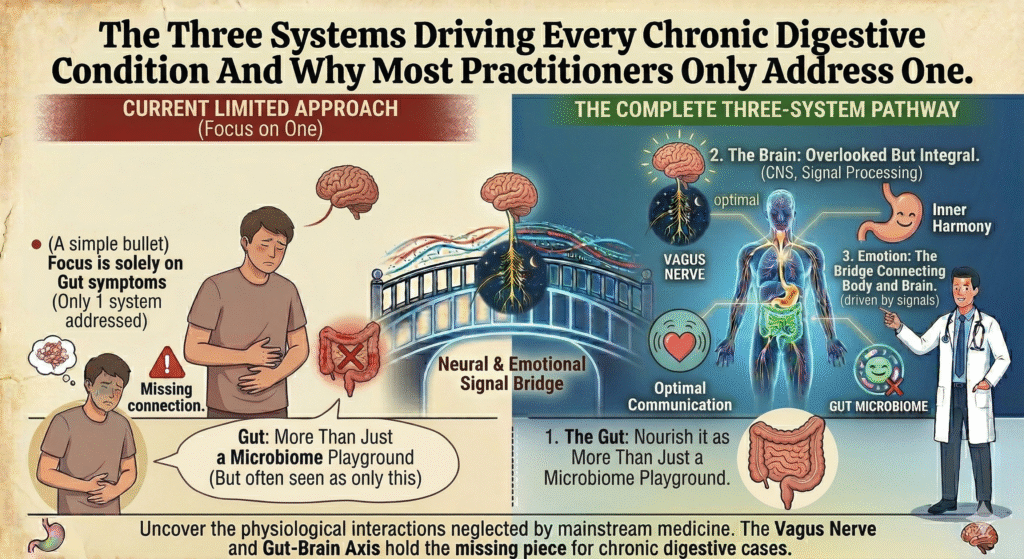
The Gut: More Than Just a Microbiome Playground
For too long, the focus has been solely on gut bacteria as the holy grail of digestive health. While the microbiome is undeniably important, neglecting the gut’s intrinsic nervous system the enteric nervous system (ENS) is a critical oversight. The ENS is often dubbed the “second brain” for a reason. It communicates with the central nervous system via the gut-brain axis, utilizing neurotransmitters like serotonin, over 90% of which is produced in the gut. Through the vagus nerve, the gut sends data to the brain. This bi-directional interaction affects mood, cognition, and even immune responses. When practitioners overlook the ENS’s role, they fail to address the neurotransmitter dysregulations that often underlie chronic digestive issues.
The emphasis should shift to acknowledging the ENS as a standalone neural network capable of operating independently of the brain. Disruptions in this network can lead to irritable bowel syndrome and other chronic digestive disorders. Addressing only bacterial imbalances without considering ENS signaling results in temporary relief but no lasting solution. Understand this: without recognizing the gut’s other roles, therapeutic efforts miss the mark.
The Brain: Overlooked But Integral
Dysregulation of the nervous system is another often-ignored contributor to gut dysfunction. When stress activation becomes chronic, the body’s fight-or-flight response mediated by the sympathetic nervous system disrupts digestive efficiency. But the more insidious issue lies in the polyvagal theory, which posits that the vagus nerve connecting the brain to the gut regulates digestive functions. If the vagus nerve’s function is impaired, the body remains in a heightened state of arousal, impacting gut motility and barrier function.
Research underlines the vagus nerve’s role in modulating intestinal permeability. A compromised vagal tone is implicated in conditions like leaky gut syndrome. When the nervous system is trapped in sympathetic dominance, the restorative functions of the parasympathetic branch regulated by the vagus nerve are impeded. This leads to persistent inflammation and poor digestive health. Ignoring the nervous system’s sovereignty in gut conditions keeps solutions superficial at best.
We must recognize that digestive disorders are as much about the brain as they are about the gut. The nervous system’s oversight is not just complementary; it is foundational.
Emotion: The Bridge Connecting Body and Brain
Lastly, emotional patterns influence gut health through pathways that are biological, not merely psychological. Stress and emotional dysregulation alter gut function via the hypothalamic-pituitary-adrenal (HPA) axis. Cortisol, released during stress, disrupts the gut lining and alters microbiota composition, escalating inflammatory responses. The interplay between emotional states and the gut is mediated by measurable biochemical processes, not subjective feelings.
The gut-brain axis acts as a conduit through which emotional and physical stressors express themselves as physical symptoms. It’s a bidirectional highway facilitated by the release of cytokines and activation of the vagus nerve. Conditions such as Crohn’s disease and ulcerative colitis have an emotional dimension directly linked to stress-induced changes within the gut microbiome. When only the physical gut symptoms are managed without addressing emotional connectivity comprehensive management remains elusive.
Those who dismiss emotional patterns as secondary misjudge the complexity of chronic digestive disorders. It is in understanding the interrelatedness of these systems that we grasp the true nature of these conditions.
Chronic digestive conditions are not isolated gut issues. They are symphonic misalignments involving the gut, the brain, and emotional patterns. Addressing just one element fails to appreciate their interconnectedness, an oversight that contributes to chronicity. True clinical understanding requires us to move beyond the reductionist paradigm. The complete picture lies in acknowledging the span of these networks.