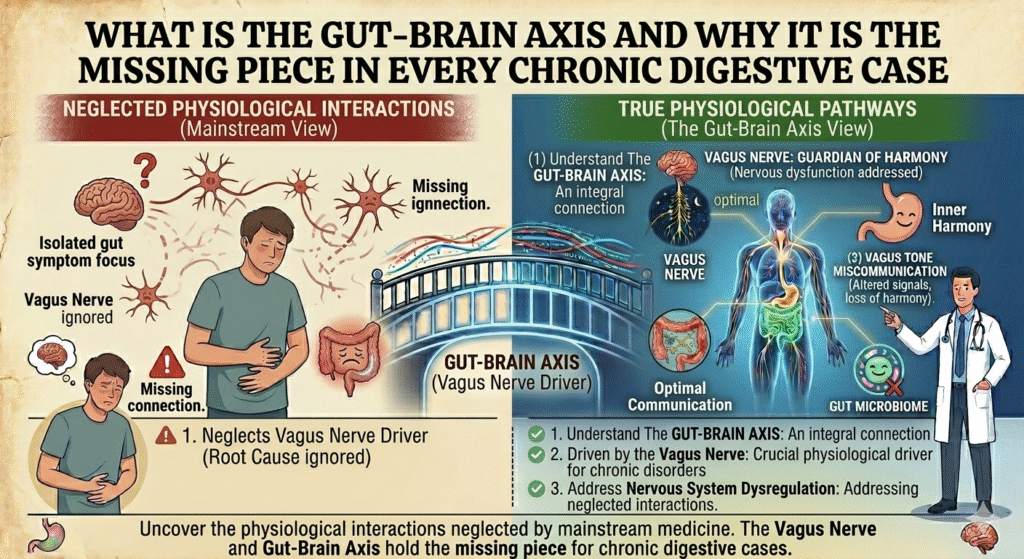
The myth that digestive issues are solely a product of diet and lifestyle is pervasive and misleading. It’s a narrow view that has failed countless patients. In truth, the core of chronic digestive disorders lies at the intersection of the gut & nervous system. The gut-brain axis, involving the vagus nerve as a major player, holds the key to understanding these conditions beyond the simplistic “you are what you eat.” When food alone doesn’t solve the problem, it’s time to look deeper into the interactions between your gut and nervous system.
The Vagus Nerve: The Master Regulator of Gut-Brain Communication
The vagus nerve, the longest cranial nerve in the body, is the conduit for the two-way communication between the gut and brain. It orchestrates autonomic control of gut functions through the enteric nervous system, often referred to as the “second brain.” This vast network doesn’t just mimic the central nervous system; it communicates directly with it. The release of acetylcholine by the vagus nerve modulates inflammation in the gut, a process critical in disorders such as Irritable Bowel Syndrome (IBS). Without an effectively functioning vagus nerve, gut inflammation spirals, immune responses malfunction, and digestive symptoms persist or worsen. Viewing digestive issues through a vagus nerve-centric lens allows for an understanding of how these symptoms are exacerbated or mitigated, a perspective that is woefully underrepresented in most clinical settings.
Polyvagal Theory: The Interaction of Emotional Patterns and Gut Dysfunction
Polyvagal theory offers a framework that surpasses traditional approaches, identifying the role of the vagus nerve in emotional regulation and its direct impact on gut physiology. When stress and emotional dysregulation occur, the vagus nerve alters its signaling, leading to disruptions in gut motility and secretions. Specifically, the dorsal vagal complex can trigger a shutdown response, reducing gut function to conserve energy under perceived threat. Such physiological states are not mere psychosomatic symptoms; they are tangible disruptions of the gut brain axis. In chronic digestive cases, addressing this dysregulation demands more than psychological interventions—it calls for a physiological recalibration that factors in the gut’s autonomic control.
Enteric Nervous System: The Unsung Player in Chronic Digestive Disorders
The enteric nervous system (ENS) is comprised of over 100 million neurons embedded within the gut lining, controlling local reflexes independently of the brain. This system acts as a local governance of gut function, influencing digestive processes through neurotransmitters like serotonin and dopamine, typically associated with the central nervous system. These neurotransmitters govern not just mood but also gut peristalsis and enzyme secretion. Dysfunction in this system doesn’t just account for gut symptoms; it disrupts the entire gut-brain axis, affecting systemic health. Pathways involving the serotonin transporter (SERT) can result in either slowed motility or accelerated transit, manifesting as constipation or diarrhea when imbalanced. The clinical misunderstanding of the ENS’s autonomy leads to futile treatments targeting only symptoms, overlooking the intricate choreography of neural signals that regulate the gut.
The gut-brain axis, underscored by the influential reach of the vagus nerve, is a clinical reality, not a wellness breakthrough. Chronic digestive issues can’t be resolved by dietary changes alone; they demand an understanding of the sophisticated neural interplay at the heart of our physiology. Addressing the gut & nervous system as a unified entity redefines the approach to treatment, grounded in science, leading to true resolution of chronic symptoms.
**Meta Description:**
The gut-brain axis, driven by the vagus nerve, is crucial in understanding chronic digestive disorders. Uncover the physiological interactions neglected by mainstream medicine.